“Lana,” a woman I interviewed who asked that her real name not be used, lives with mitochondrial disease and is an active member of a private Facebook group of people who share her diagnosis. Some of the members have become experts in drug interactions particular to “mito” and offer guidance to others based on their […]
pt/doc co-care
Rare Disease Day
Today is Rare Disease Day, when we honor the millions of people who teach us what it’s like to live at the edges of the known world of medicine.
Imagining better outcomes for T1D with #MakeHealth
This post originally appeared on Diabetes Mine. Forty-five makers, thinkers, designers and doers gathered in Cincinnati for a two-day meeting to kick off “Phase Zero” of a new initiative to imagine a new system of care for people living with Type 1 diabetes (T1D). The best way I can describe the group is that everyone […]
“We just flipped a switch.”
“At one level, we just flipped a switch. It wasn’t a complicated, multi-faceted, variegated intervention. All we did was open up the doctor’s notes… Out of that came a cascade.” – Tom Delbanco talking about OpenNotes and how a seemingly simple change — allowing patients to view clinicians’ notes from their visits — is having […]
False boundaries in health care
Clayton Christensen gave a talk at last week’s SMARTHealthIT board meeting on, as he put it, how people think. I was absorbed by his storytelling, so only wrote down a few concepts: We make assumptions based on false correlations (and we should guard against that tendency). Data and maps are verbs, not nouns, and they never tell the […]
Secret questions, naked truths
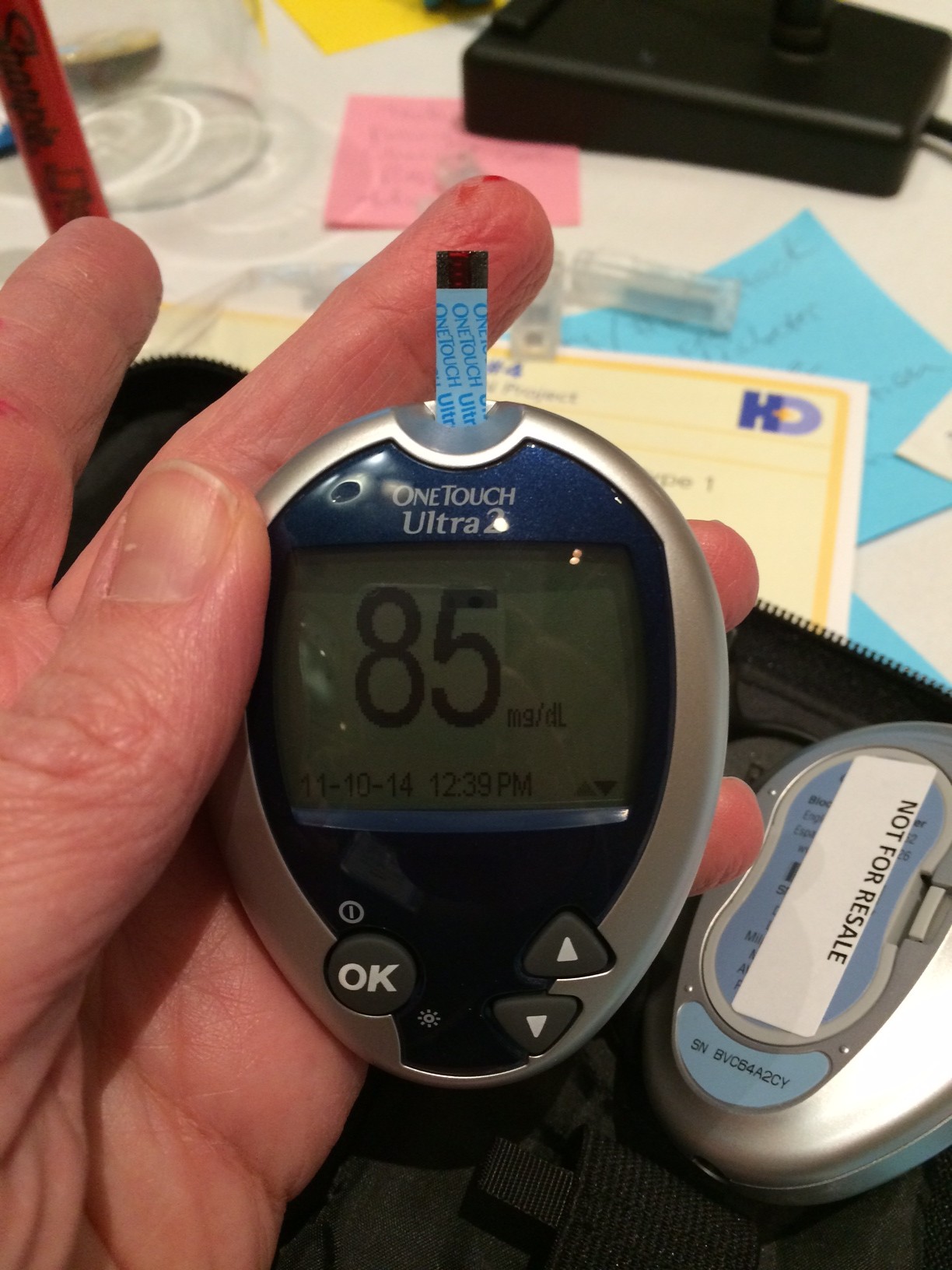
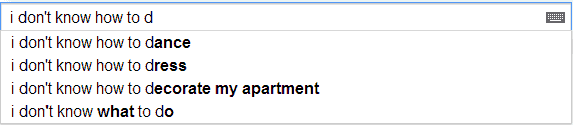
My prepared remarks for the Quantified Self Public Health Symposium (here are some notes from the event): You know when you type the first few words of a query and Google suggests the rest based on what thousands of other people have typed next? There’s a Twitter account called Google Poetics that takes those suggested phrases […]



Recent Comments